Jeremy Lasek – PHAA
Australia has passed another important milestone in its ever-accelerating vaccination rollout, administering more than 16 million COVID-19 vaccine doses and tracking towards meeting the agreed National Cabinet thresholds of 80% fully vaccinated, to start freeing us up from restrictions before the end of the year.
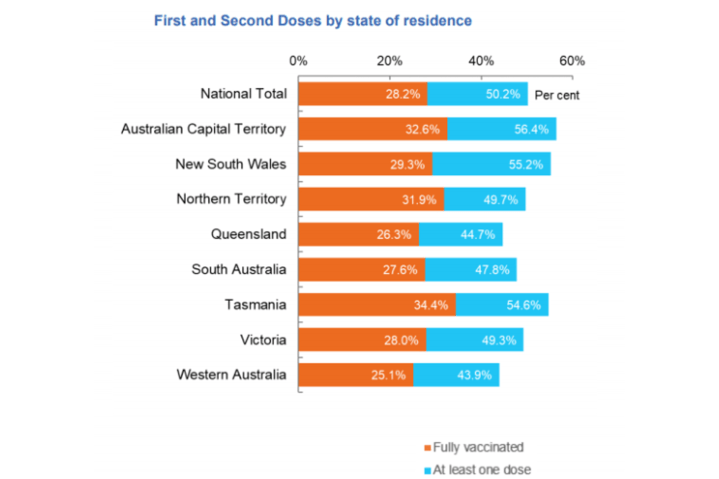
Since the start of vaccinations in late February, 50.2% of people over the age of 16 (>10.3 million) have received at least one dose while 28.2% (>5.8 million) are now fully vaccinated. There is, however, a growing discussion about whether vaccines should be mandated.
Victorian fruit and vegetable processor SPC became the first Australian company to mandate vaccines for its 450-strong onsite workforce and for visitors from November. Since then, Qantas has joined the organisations signalling the requirement for staff to be vaccinated.
Others believe mandating COVID-19 vaccinations should be a last resort.
In an article she co-authored for the Sydney Morning Herald, PHAA member, Professor Julie Leask, an adviser to the World Health Organization on improving vaccination uptake, and Professor Jane Williams, Public Health ethicist, urged caution in ‘jumping to mandates without exhausting reasonable options’.
‘Poorly thought up ‘pop-up’ mandates from any sector will lead to chaos and the kinds of harms that compete with the ultimate aim of vaccination – human wellbeing,’ the article says. ‘Community-based mandates have a slightly different aim to occupational ones – to get high vaccination coverage. Yet they suggest that people have to be forced, rather than accepting that for the most part people want to do the right thing.
They suggest employers who want to ensure high vaccine coverage in the workplace should provide vaccination at work, paid time off for all staff to receive it and, if necessary, recover from it.
‘The World Health Organization sets out pre-requisites for vaccine mandates to be justifiable. The mandate must be necessary to achieve an important public health goal that can’t be achieved by using other reasonable means (e.g. mask wearing, physical distancing, testing). The vaccine must be safe, and it must be effective. As well as protecting the individual, it must also be able to prevent spread to some degree so that it protects the public. There must be enough vaccine for everyone who wants it, and mandating the vaccine must not undermine public trust. These last two points are where the problems of mandating vaccine lie in Australia.’ they wrote.
Providing the contrary view, Professor of bioethics, Peter Singer, in making the case for compulsory vaccinations, using the example of Victoria becoming the first jurisdiction in the world to introduce the mandatory wearing of seatbelts in cars in 1970.
‘The legislation was attacked as a violation of individual freedom, but Victorians accepted it because it saved lives. Now most of the world has similar legislation. I can’t recall when I last heard someone demanding the freedom to drive without wearing a seat belt,’ Professor Singer said.
He lamented that the move to introduce compulsory vaccinations in one of Australia’s near neighbours came too late.
‘This past February, when the Indonesian government became the first to make vaccination mandatory for all adults, the real tragedy was not that it was violating the freedom of its citizens, but that richer countries did not donate the vaccines it needed to implement the law.
‘As a result, Indonesia is now the epicentre of the virus and tens of thousands of unvaccinated Indonesians have died.’
According to PHAA CEO Adjunct Professor Terry Slevin, there needs to be an active discussion on vaccination policy as we approach 2022. “Until such time that the supply shortage is resolved and everyone who wants to be vaccinated has easy access to the vaccine, the greatest possible effort needs to be committed to actively ensuring open honest and clear evidence about the benefits and the risk with any recommended vaccine is effectively communicated”.
“This is a public health policy that should not be left to individual employers. Clear guidance and leadership need to be provided from government based on the best available evidence and advice from those with the relevant expertise” he said.
He also supported Professors Leask and Williams recommendation “meaningful and transparent consultation and planning now will benefit trust in public health and vaccination that will pay future dividends.”
Photo credit: Australia’s COVID-19 Vaccine Roadmap – Vaccinations by location, data as at 18 August 2021.

Leave a Reply